Hypoglycaemia In Children With Diabetes
Hypoglycaemia In Children With Diabetes
Hypoglycaemia happens when the blood glucose level is less than 4 mmol/L, or where your child has symptoms of hypoglycaemia at a level close to this.
Key points about diabetes and hypoglycaemia
- hypoglycaemia is the most common acute complication of type 1 diabetes
- treatment is urgent
- the amount of glucose needed to treat hypoglycaemia depends on your child's size, insulin regimen, recent insulin dose and recent exercise
- hypoglycaemia can be mild, moderate or severe
- your child can have glucose levels mostly within the target range of 4 to 8 mmol/L without risking severe hypoglycaemia
Tamariki (children) and rangatahi (young people) need urgent treatment for hypoglycaemia.
What is hypoglycaemia?
Hypoglycaemia happens when the blood glucose level is low enough to cause signs or symptoms, including impaired brain functioning. These can expose your child to possible harm.
The level used to identify and treat hypoglycaemia in your child with diabetes is less than 4.0 mmol/L.
See a short video about hypoglycaemia at the Starship Child Health website.
What are the main causes of hypoglycaemia?
- too much insulin
- missed or delayed meals, or eating too little carbohydrate at meals
- exercise, without decreasing the insulin or without eating additional carbohydrate
- illness which causes vomiting and/or diarrhoea
- alcohol intake
What are the symptoms of mild to moderate hypoglycaemia?
Symptoms of mild to moderate hypoglycaemia may include one or more of the following:
- feeling hungry
- looking pale
- feeling shaky
- having a headache
- feeling dizzy
- feeling sweaty
- a change in behaviour or irritability
- a lack of concentration
- crying
- confusion
- blurred vision
Babies and young children may not say that they are feeling unwell.
In younger children, change in behaviour is the most common sign. They may be unusually quiet, grizzly, unhappy or hungry. If you notice any of these symptoms in your child, or if you are concerned about your child's behaviour for any reason, it is important to check their glucose levels.
If using intermittently scanned continuous glucose monitoring, for example Freestyle Libre-1, it is important to check your child's blood glucose level with a finger-prick. This will confirm either:
- a hypoglycaemia episode
- a trend indicating a rapid fall in glucose levels
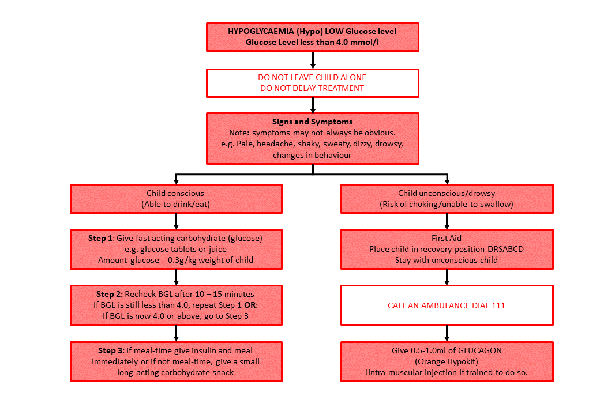
What is the treatment for hypoglycaemia?
You might find a hypoglycaemia flow chart (PDF, 80KB) helpful for what to do if your child has hypoglycaemia.
Treatment is urgent.
The amount of glucose needed to treat hypoglycaemia depends on your child's size, insulin plan, recent insulin dose and recent exercise.
Confirm hypoglycaemia by checking glucose level
If there are any signs or symptoms of hypoglycaemia, confirm hypoglycaemia by checking glucose level.
You may detect hypoglycaemia (less than 4 mmol/L) during a routine glucose level check.
It is important to do a finger prick check if:
- using intermittently scanned continuous glucose monitoring (Freestyle Libre-1)
- using a continuous glucose monitor and your child's symptoms do not match the sensor glucose reading
- using a continuous glucose monitor (CGM) and your child is not experiencing any symptoms but the CGM is reading as less than 4.0 mmol/L
Step 1: Treatment with glucose (using formula of 0.3g per kilogram)
Amount of glucose to give:
- give enough glucose to increase the glucose level quickly to 4.0 mmol/L or above, ut not so much that it will result in hyperglycaemia
- you can use the following formula - 0.3g/kg of your child's current weight
Examples of using the formula (0.3g/kg of your child's current weight):
- if your child is 24kg, give 7g of glucose
- if your child is 50kg, give 15g of glucose
Examples of glucose include:
Juice drink
- for example, Twist ™ 13 to 17g per 125ml box of juice
- or Just Juice Splash™ 6.3g for child weighing less than 20 kg
Glucose tablets
- glucose tablets (3 to 4g each, depending on the make of the tablets)
- don't give tablets if your child is under 5 because they might choke
Other options
- 5 to 6 Mentos for older children over 50kg
Step 2: Re-check blood glucose level
Re-check blood glucose level after 10 to 15 minutes.
Symptoms should go away within 10 to 15 minutes of step 1 treatment.
If blood glucose level is less than 4 mmol/L at the 10 to 15 minute check, repeat step 1 treatment.
If blood glucose level is greater than 4 mmol/L, move to step 3.
Step 3: Have snack or meal
- give 10 to 20g 'snack' of long-acting carbohydrate or
- if meal is due, give insulin followed by meal straight away
Snack examples include (adjust for the age and size of your child):
- a slice of bread
- 200ml milk
- an apple or half a banana
- 2 plain biscuits
Your child will not always need a follow-up carbohydrate snack - see note for children on insulin pump therapy.
A note for those on insulin pump therapy and hybrid closed loop
Children on insulin pump therapy will often NOT need the follow up or long-acting carbohydrate, unless their glucose level is less than 3 mmol/L.
Often, children on pumps also need less carbohydrates than those on injections to treat hypoglycaemia. This is especially true for children on either:
- hybrid closed loop (HCL) or
- predictive low glucose suspend insulin pump therapy (for example, Tandem T-slim Basal IQ, or Control IQ, or Medtronic 780G, or predictive low glucose suspend)
If the system is suspending insulin delivery because it is predicting a low glucose level, do NOT treat with carbs. Only treat glucose levels confirmed less than 4 mmol/L.
If your child is on HCL, they will likely NOT need a snack to prevent lows when exercising.
Night-time lows
Hypoglycaemia at night is more likely to happen after increased levels of activity during the day or if your child has eaten less or is unwell. It is important to talk with your child's paediatric diabetes team for individual advice for your child.
Some strategies to reduce the risk of hypoglycaemia at night are:
- aiming for glucose levels of 4 to 8 mmol/L during the day, at bedtime and overnight is the best way to avoid hypos at night
- if you think there may be an increased risk of hypoglycaemia, check glucose levels around 1am and treat glucose levels less than 4 mmol/L
- reducing daytime insulin doses if you know there will be a lot of exercise during the day
- reducing evening basal and possibly also rapid acting insulin doses if there has been a lot of exercise in the evening
- utilising temporary basal rate or temporary targets if using an insulin pump
What is hypoglycaemia unawareness?
Hypoglycaemia unawareness (also called impaired awareness of hypoglycaemia) is when a blood glucose check shows hypoglycaemia but your child is not aware of it.
Toddlers and young children who are newly diagnosed may not sense hypoglycaemia very effectively. Or, they may not be able to explain how they are feeling. Detecting hypoglycaemia in these particular groups relies solely on others. Children need support to learn how to recognise and describe their hypoglycaemia symptoms.
In older children and teens, hypoglycaemia unawareness can develop following frequent hypoglycaemia episodes. This is a dangerous condition where hypoglycaemia can happen quickly and the risk of severe hypoglycaemia is increased.
What is severe hypoglycaemia?
Severe hypoglycaemia is when a person is so confused or drowsy they are unable to manage low glucose levels themselves or are unconscious and will need the help of another person.
The symptoms of severe hypoglycaemia include the following:
- blood glucose level less than 4 mmol/L
- extreme drowsiness and disorientation or confusion
Someone with severe hypoglycaemia may also:
- have slurred speech and lack of coordination
- be unconscious
- have a seizure
Do NOT give your child food or drink if they are unable to swallow as this might lead to choking.
How is severe hypoglycaemia managed?
Actions for severe hypoglycaemia
- call for help
- place your child in the recovery position and make sure their airway is clear
- call for an ambulance (dial 111 within New Zealand - use the appropriate emergency number in other countries) and tell them it is a child with diabetes having a severe hypo
- administer Glucagon (Glucagen™) - see below for instructions
The symptoms of severe hypoglycaemia are a blood glucose level less than 4 mmol/L and extreme drowsiness and disorientation or confusion. Someone with severe hypoglycaemia may also:
- have slurred speech and lack of coordination
- be unconscious or passed out
- have a fit or convulsion
In severe hypoglycaemia, you or someone else needs to make a judgement about whether it is safe to treat your child with sweet foods or drink. Your child needs to be conscious and cooperative enough to be able to swallow. If your child is too drowsy or disoriented to understand and follow instructions, then they shouldn't have anything by mouth. This is to prevent possible choking.
How do I give a glucagon injection with the GlucaGen™ hypokit for severe hypoglycaemia?
The GlucaGen™ hypokit contains a synthetic form of glucagon. Only parents and others who have been appropriately trained can give a glucagon injection.
What happens during recovery from severe hypoglycaemia following glucagon injection?
- your child or teen should generally wake within 10 to 15 minutes of receiving the glucagon - if your child has had a convulsion, it should usually be short and does not cause permanent damage
- when your child is awake, give sips of sweet fluid (such as juice drink, lemonade)
- severe hypoglycaemia can cause vomiting and/or severe headache - continue to offer sips of sweet fluid until your child is able to take small amounts of long-acting carbohydrate (such as crackers)
- monitor the blood glucose levels every 15 minutes
- your child will need close observation for the next 2 hours - this may need to happen in hospital
- contact your diabetes team for advice
- your child is at risk of further episodes of hypoglycaemia unless doses are adjusted
What if my child has repeated hypoglycaemia, or is unwell and can't eat or drink?
Find out when to use mini-dose glucagon for children with diabetes.
What can cause fear of hypoglycaemia?
Symptoms of hypoglycaemia can be distressing for children and young people, and parents. This can lead to a significant fear or avoidance of hypoglycaemia. This fear can increase anxiety, cause interrupted or poor sleep patterns and reduce a person's quality of life (both children and parents).
Fear of hypoglycaemia can also lead to people preferring higher glucose levels which comes with other risks and will NOT necessarily prevent hypoglycaemia. Talk to your diabetes team so that you and your child can be supported.
Find out about possible complications in children with diabetes.
See more KidsHealth content on diabetes
This page last reviewed 15 February 2023.
Do you have any feedback for KidsHealth?
If you have any feedback about the KidsHealth website, or have a suggestion for new content, please get in touch with us.
Email us now