Video by Clearly Health [1], Canada.


Type 1 diabetes is a lifelong condition where the level of glucose in the blood is too high due to a lack of insulin.
You might find it helpful to watch the animated video about diabetes and the body at the top of the page.
Type 1 diabetes happens when the insulin making cells can't make enough insulin.
Without insulin, blood glucose levels are high but the body can't use any of the glucose for energy.
When the body can't use glucose, it breaks down fat and protein for energy. This process produces ketones. In large amounts, ketones can make a person very unwell and cause:
Glucose is the main source of energy in our bodies. It is mostly made when our bodies break down the carbohydrates that we eat or drink.
Glucose is absorbed from the gut into the blood stream.
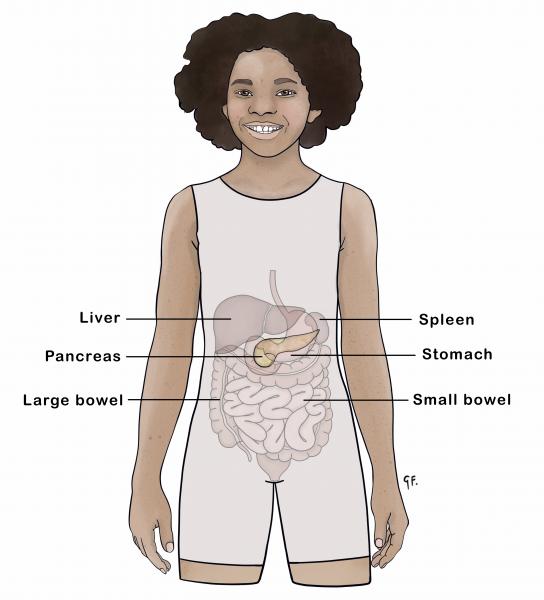
Insulin is a hormone produced by special cells called beta cells in the pancreas. The pancreas is an organ in the abdomen, behind the stomach.
Insulin allows the glucose from the bloodstream to move to the cells in the body. From there it's used as fuel for energy.
There are 2 main types of diabetes affecting tamariki and rangatahi - type 1 and type 2 diabetes.
See the KidsHealth page on type 2 diabetes [2].
Other types of diabetes are rare in tamariki and rangatahi.
Type 1 diabetes just happens. There is nothing you did to cause it. There is nothing you could have done to prevent it.
Type 1 diabetes is not caused by eating too much sugar.
You can't catch diabetes or spread it to anyone else.
Health professionals do not fully understand why people develop type 1 diabetes.
Diabetes is triggered by an unknown environmental factor in people who are born with a genetic tendency to diabetes.
The body's immune system (infection-fighting system) normally protects us from infections. Once diabetes is triggered by the unknown environmental factor, the immune system starts to produce antibodies. These antibodies attack and destroy the insulin producing cells in the pancreas.
This process can continue for weeks or even years before the symptoms of diabetes start. This is because the symptoms happen when 90% of the cells are destroyed.
If your child has any of the symptoms of type 1 diabetes, please seek medical advice as soon as possible.
Once your child has symptoms, they may become very sick very quickly.
The combination of high blood glucose levels and high ketone levels can cause severe dehydration and loss of salts from the body.
This is called 'diabetic ketoacidosis' or DKA. It is life threatening.
The development of type 1 diabetes is a medical emergency, and your child will need to go to hospital.
Doctors and nurses will look after you and your child. They will do some blood tests to confirm the diagnosis of diabetes.
Doctors and nurses will start treatment with insulin to reverse the symptoms and make your child feel better.
Your child cannot take insulin by mouth. The medical team will decide the best way to give insulin - either by injections or by infusion into a vein.
You and your child will stay in hospital for a few days after the diagnosis to receive further education and support. You will also meet your new diabetes team. They will help you when you are managing diabetes at home. They will also see you for regular clinic visits.
Tamariki with type 1 diabetes need insulin to replace the insulin that the body cannot make anymore.
Insulin is a hormone which you cannot take by mouth. You must inject it into the layer of fat under the skin. You can do this by injections or using an insulin pump.
Injections

Insulin pump
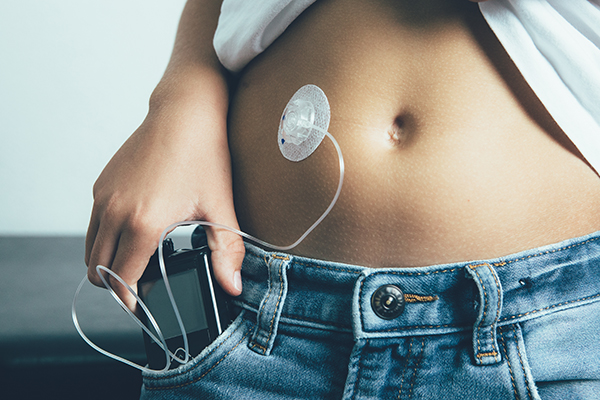
People with type 1 diabetes cannot survive without insulin treatment.
At first, your diabetes team will tell you how much insulin you need. They will teach you and your family how to adjust and calculate the insulin dose.
See KidsHealth's page on giving insulin to children with diabetes [3].
The aim is to keep blood glucose levels within target range (4 to 8 mmol/L).
Monitoring your blood glucose levels allows you and your diabetes team to adjust the insulin doses.
You can do this by:
See KidsHealth's page on glucose monitoring in children with diabetes [4].
A child or young person with type 1 diabetes needs to eat a healthy diet, just like those without diabetes.
They need to regularly eat carbohydrates for growth and development, just like those without diabetes.
See KidsHealth's page on type 1 diabetes in children - general guidelines on nutritional management [5].
See KidsHealth's page on healthy eating for children with diabetes [6].
Physical activity is part of a healthy lifestyle.
Tamariki and rangatahi with type 1 diabetes can exercise safely and join in PE classes and team sports.
Aiming for at least 60 minutes of physical activity each day is important for all tamariki and rangatahi.
To avoid low blood glucose levels, tamariki may need extra carbohydrates and adjustment of insulin doses.
It's important to understand what can happen with blood glucose levels during and after exercise. It's also important to have a plan to manage it.
See KidsHealth's page about how children with type 1 diabetes can exercise safely [7].
See KidsHealth's page about encouraging children and young people with diabetes to be active [8].
The amount of insulin needed depends on the amount of carbohydrates and the amount of physical activity.
There is a lot to learn about how to care for a child or young person with diabetes.
This learning involves the whole whānau and community. It involves people involved in your child's life such as school staff, friends, neighbours, sports coaches etc.
Education and learning about type 1 diabetes is an ongoing process.
It's important to monitor blood glucose levels and try to keep them within target range (4 to 8 mmol/L) even if your child is feeling 'OK' at the moment.
High blood glucose level over a long period of time leads to serious complications. Screening is important to find any possible developing complications early.
Possible complications include:
See KidsHealth's page on possible complications in children with diabetes [9].
You can minimise long-term risks and complications by:
Be supportive and understanding but make sure your child gets the treatment they need.
Go to regular appointments with the diabetes team.
Talk to your child's school or early education centre about the support available. This may be through the school or the Ministry of Education.
See KidsHealth's page about creating a safe environment for children with diabetes at school [10].
Reach out to the local and online communities and support groups, for example:
Help your child maintain long-term health and minimise the risk of diabetes complications. You can do this by:
The content on this page has been approved by the Clinical Network for Children and Young People with Diabetes, Paediatric Society of New Zealand.
The photos of injection and insulin pump are from iStock.
Illustration showing pancreas and surrounding organ by Dr Greta File. Property of KidsHealth.
This page last reviewed 14 November 2023.
Email us [21] your feedback
Links
[1] http://www.clearlyhealth.com
[2] https://kidshealth.org.nz/type-2-diabetes-children-overview
[3] https://kidshealth.org.nz/giving-insulin-children-diabetes
[4] https://kidshealth.org.nz/glucose-monitoring-children-diabetes
[5] https://kidshealth.org.nz/type-1-diabetes-children-general-guidelines-nutritional-management
[6] https://kidshealth.org.nz/healthy-eating-children-diabetes
[7] https://kidshealth.org.nz/how-children-type-1-diabetes-can-exercise-safely
[8] https://kidshealth.org.nz/encouraging-children-young-people-diabetes-be-active
[9] https://kidshealth.org.nz/possible-complications-children-diabetes
[10] https://kidshealth.org.nz/creating-safe-environment-children-diabetes-school
[11] https://www.diabetes.org.nz/
[12] https://www.diabetesfoundationaotearoa.nz/
[13] https://kidshealth.org.nz/tags/diabetes
[14] https://starship.org.nz/diabetes-resources/
[15] https://kidshealth-old.schn.health.nsw.gov.au/caring-diabetes-children-and-adolescents-4th-edition-2021
[16] https://diabetes.org/
[17] https://www.ispad.org/page/ISPADGuidelines2022
[18] https://kidshealth.org.nz/node/1865?language=zh-hans
[19] https://www.diabetes.org.nz/youth
[20] https://www.diabetes.org.nz/branches/
[21] https://kidshealth.org.nz/contact?from=http%3A%2F%2Fkidshealth.org.nz%2Fprint%2F2857%3Flanguage%3Dzh-hans